Knowing the difference between a healthy socket vs dry socket after a tooth extraction can save you from days of unnecessary pain — or help you catch a real problem before it gets worse. You just had a tooth pulled, the numbness is wearing off, and now you are staring at your phone, wondering: Is this normal healing, or is something wrong?
For millions of people each year, telling apart a healthy socket vs dry socket is one of the most confusing and anxiety-inducing parts of dental recovery. Both involve soreness, both look a little alarming at first, and neither comes with a label. The difference, however, is significant — one is your body doing its job perfectly, and the other is a painful complication that needs dental attention fast.
This guide breaks down the healthy socket vs dry socket comparison across 7 clear, practical differences so you know exactly what to watch for, what is normal, and when to pick up the phone and call your dentist.
What Happens Inside Your Mouth After a Tooth Extraction?
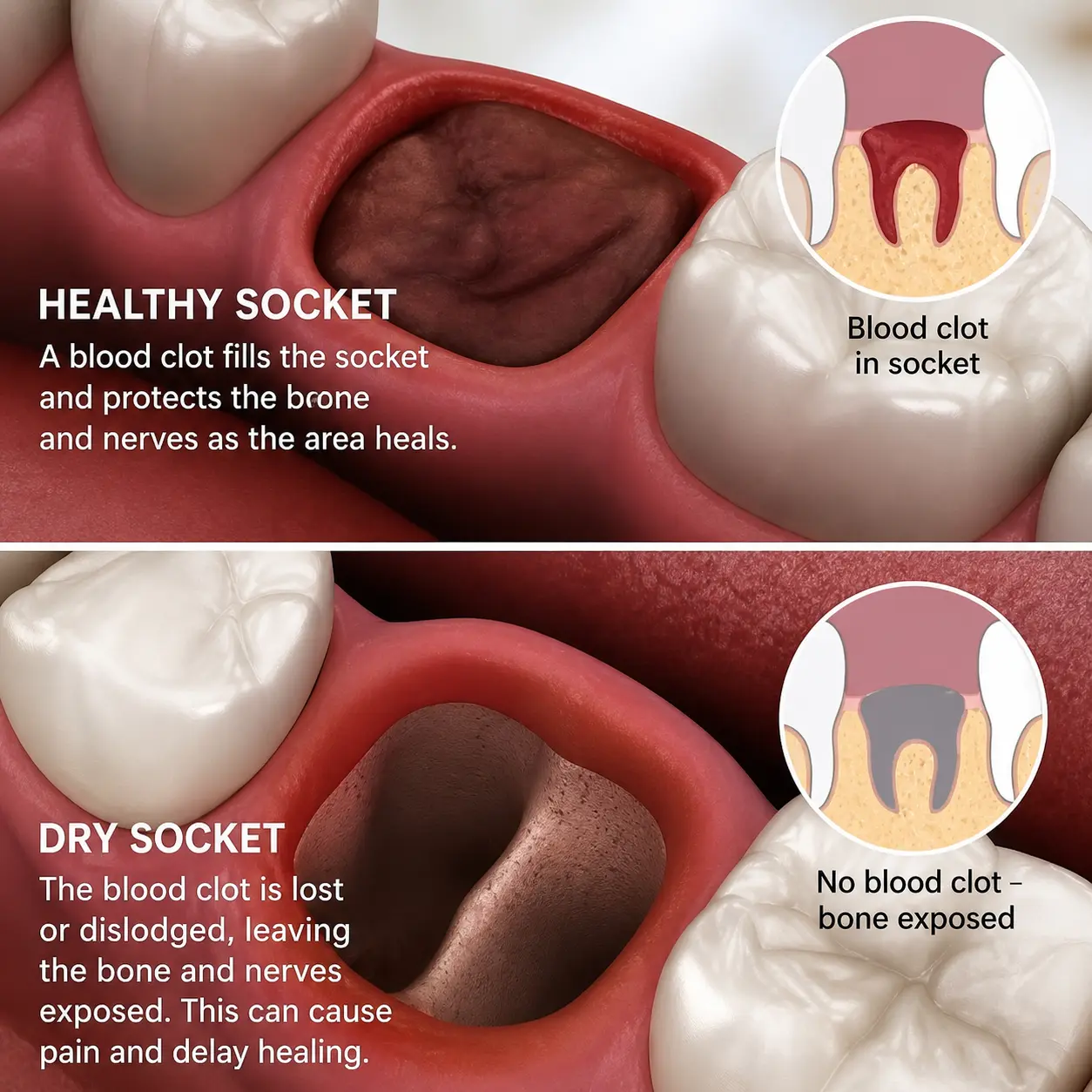
After a tooth is removed, your body immediately begins repairing itself. Understanding the healthy socket vs dry socket distinction starts here — with what happens in that socket right after extraction. A blood clot forms inside the empty socket — the hollow space left behind in your jawbone — and this clot acts as a natural bandage. It shields the exposed bone and nerve endings from air, food, bacteria, and anything else that enters your mouth.
Over the next few days, that clot slowly transforms into new tissue called granulation tissue. Then, over weeks, the bone underneath begins to fill in. When this sequence runs smoothly, you have a healthy socket. When the clot is disrupted or never fully forms, you end up with a dry socket instead — and that is where the pain really begins.
Think of the blood clot as the foundation of your entire healing process. Lose it, and everything built on top of it collapses.
Fact #1: According to the Cleveland Clinic, this healing process follows a predictable biological sequence: clot formation first, then tissue regeneration, and finally new bone growth — a sequence that only completes properly in a healthy socket.
What Does a Healthy Socket Look Like?
A healthy socket has a dark red or maroon-colored clot sitting inside it during the first day or two. In a healthy socket vs dry socket comparison, this dark clot is the single most important visual clue — its presence signals that healing is on track. As days pass, the socket appears smaller because new gum tissue gradually closes over the area.
You may also notice white or yellowish tissue forming around the edges of the clot. This is called granulation tissue — it is a completely normal sign that healing is underway. Many people mistake it for an infection, but it is actually a good sign.
What you should see in a healthy socket:
- A dark, clot-like covering over the hole
- No visible bone inside the socket
- Tissue slowly closing over the site over 1–2 weeks
- Pain that decreases a little more each day
Fact #2: A healthy tooth extraction site appears deep red with white gelatinous tissue forming over the socket as healing progresses, according to dental health sources.
What Is Dry Socket — and Why Does It Happen?
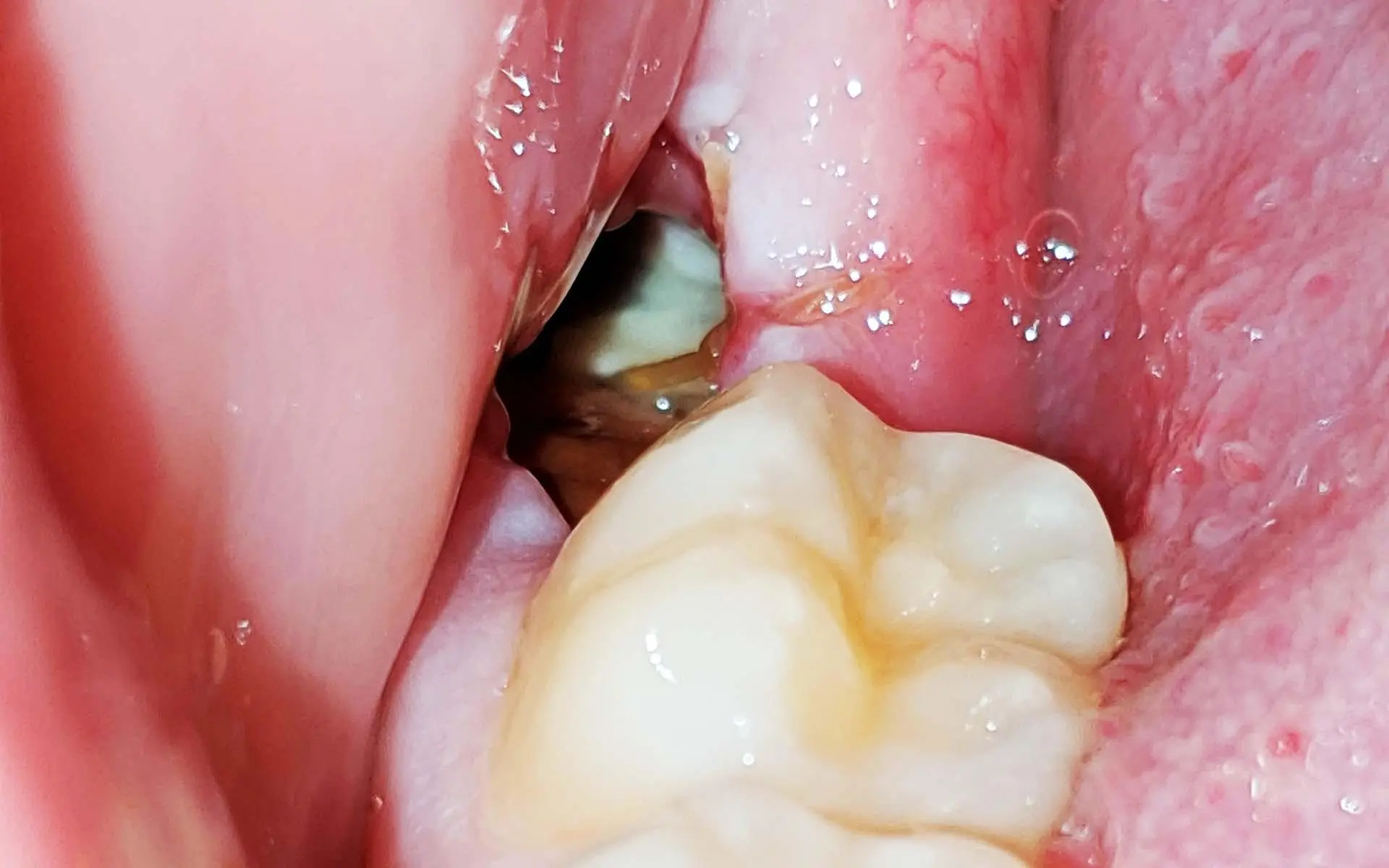
Dry socket, medically known as alveolar osteitis, occurs when the protective blood clot either fails to form properly or gets dislodged before the wound heals. Without that clot, the bone and nerve endings inside the socket are left completely exposed.
This exposure means air touches the nerves directly. Food particles can fall in. Bacteria can settle inside the open hole. The result is intense, escalating pain that over-the-counter painkillers often cannot manage well.
Fact #3: Dry socket affects approximately 2% to 5% of all routine tooth extractions, according to the Cleveland Clinic. However, that number is significantly higher for wisdom tooth removals, where it can be more common due to the complexity of the procedure.
Fact #4: A 2022 study found the combined incidence of dry socket in smokers was about 13.2%, compared to roughly 3.8% in non-smokers — making tobacco use one of the most significant risk factors.
Healthy Socket vs Dry Socket: Key Differences at a Glance
Here is a quick-reference summary of the 7 most important differences between a healthy socket vs dry socket. Each one is expanded in detail in the sections below.
| # | What to Check | Healthy Socket | Dry Socket |
|---|---|---|---|
| 1 | Pain trend | Decreasing each day | Worsening after day 1–3 |
| 2 | Appearance | Dark clot, no visible bone | Open, pale/gray, bone visible |
| 3 | Smell / taste | Normal | Foul odor or bad taste |
| 4 | Swelling | Mild, subsides in 2–3 days | May persist or worsen |
| 5 | Tissue formation | White granulation tissue forming | Empty socket, no tissue coverage |
| 6 | Response to painkillers | OTC medications manage pain well | Pain often unresponsive to OTC meds |
| 7 | Healing progress | Visibly improving each day | Stalled or getting worse |
Understanding the contrast between these two conditions is really about paying attention to two things: what you see and what you feel. Let’s go through each difference in detail.
Difference #1 — How Does the Pain Compare?
Pain is the most telling difference when comparing a healthy socket vs dry socket. In a healthy socket, pain is noticeable immediately after the procedure but begins to ease within 24 to 48 hours. Each day should feel slightly better than the last. You should be able to manage the discomfort with standard over-the-counter medications like ibuprofen or acetaminophen.
With dry socket, the pattern is the complete opposite. Pain begins to intensify rather than improve, typically starting 1 to 3 days after the extraction. The pain can radiate outward from the socket — spreading toward the ear, the jaw, or even the forehead on the same side of the face. It is not subtle. Most people describe it as one of the worst toothaches they have ever experienced, and over-the-counter pain relief often does very little to take the edge off.
This escalating vs. diminishing pain pattern is the single fastest way to tell a healthy socket vs dry socket apart — no mirror required.
Fact #5: According to Medical News Today, dry socket pain typically becomes worse 3 to 5 days after an extraction — exactly when a healthy socket should be feeling noticeably better.
Difference #2 — What Does Each Socket Look Like?
This is where visual inspection becomes very useful when assessing a healthy socket vs dry socket. If you look carefully at the extraction site using a mirror and a small flashlight:
- Healthy socket: You see a dark clot covering the hole. No bone is visible. The area looks protected and “filled in.” Over time, white granulation tissue begins to form around the edges.
- Dry socket: The socket looks open and empty. You may see a whitish, gray, or pale surface at the bottom — that is exposed bone. The hole appears larger or more open than expected, and nothing is protecting the interior.
In a healthy socket, the site visibly shrinks and fills in day by day. In a dry socket, it can look the same — or worse — compared to day one. If you can see what looks like bone inside the socket, that is a strong visual indicator of dry socket and warrants an immediate call to your dentist.
Difference #3 — Does Smell or Taste Indicate a Problem?
Yes — and this is one of the less-discussed but surprisingly reliable signs when distinguishing a healthy socket vs dry socket. A healthy socket, even while actively healing, does not produce a significant or unpleasant odor. Mild discomfort is expected; a foul smell is not.
Dry socket, on the other hand, often causes noticeably bad breath or an unpleasant, bitter taste in the mouth. When the blood clot is absent, bacteria and food particles accumulate inside the exposed socket, creating an odor that regular brushing or mouthwash cannot fully resolve.
If you are maintaining good oral hygiene and still noticing a persistent foul taste or smell coming specifically from the extraction site, treat it as a warning sign worth acting on.
What Causes Dry Socket? Common Risk Factors to Know
Several behaviors and health conditions shift you from healthy socket vs dry socket outcomes. Some risk factors are within your control; others are not. Understanding them helps you make informed decisions in the days following your extraction.
Actions that can dislodge the blood clot:
- Drinking through a straw (the suction pulls the clot out)
- Vigorous rinsing or spitting in the first 48 hours
- Smoking or using tobacco products
- Eating hard, crunchy, or chewy foods too soon
- Poking the socket with a finger or a toothbrush
Health-related risk factors:
- Taking oral contraceptives containing estrogen, which can affect clot stability
- Pre-existing oral infections or untreated gum disease
- A previous history of dry socket — if you have had it once, you are more susceptible again
- Wisdom tooth extractions, especially impacted ones, carry a higher risk than simpler procedures
Fact #6: Women taking estrogen-based oral contraceptives have a statistically higher risk of developing dry socket after tooth extraction, due to the hormone’s effect on blood clot stability.
Fact #7: Complex or impacted wisdom tooth extractions carry a significantly higher risk of dry socket than routine extractions, because the procedure is more invasive and disrupts surrounding tissue.
What Is the Healing Timeline for a Normal Socket?
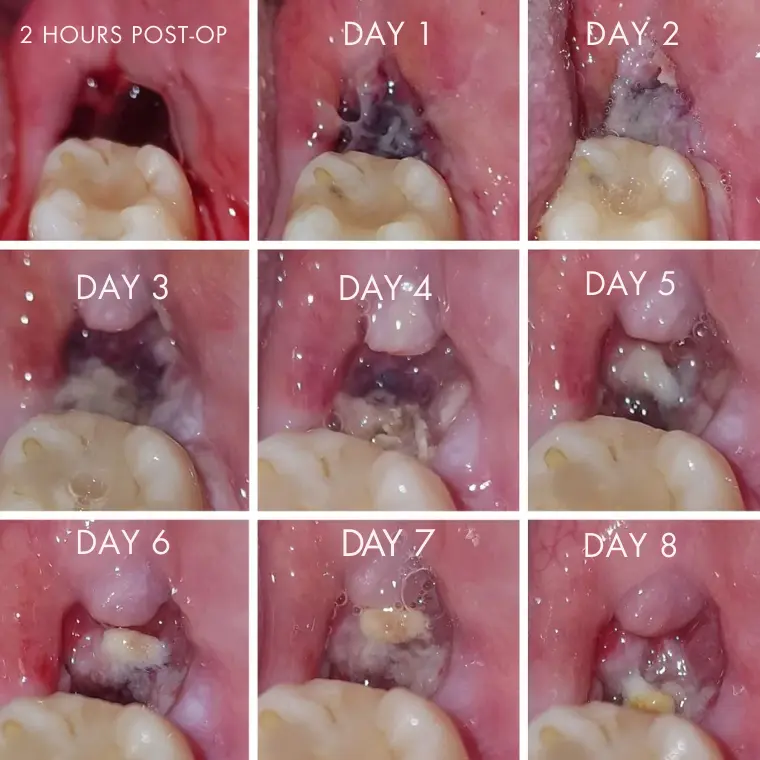
Knowing the expected timeline is another practical way to judge healthy socket vs dry socket status at home. Here is what normal recovery looks like day by day:
- Day 1–2: Bleeding slows, clot forms, swelling and mild pain are normal
- Day 3–4: Pain should begin to noticeably decrease; tissue starts forming
- Day 5: If a visible clot is still present and pain has been improving, you are most likely out of the dry socket risk window
- Week 1–2: Gum tissue closes over the socket; most discomfort is gone
- Months 2–3: Underlying bone continues to heal and fill in
Fact #8: According to dental health sources, the risk window for dry socket development is primarily 3 to 5 days post-extraction. After the five-day mark with a visible clot, the risk drops significantly.
For wisdom tooth extractions, the overall healing timeline is longer, and the risk period may extend slightly. Complete bone healing beneath the gum can take 2 to 3 months, regardless of which tooth was removed.
Healthy Socket vs Dry Socket After Wisdom Tooth Removal: Is It Different?
Wisdom tooth extractions deserve their own mention because the healthy socket vs dry socket dynamic is notably more complicated with these teeth. Wisdom teeth — especially impacted ones — sit deeper in the jaw, require more tissue disruption to remove, and leave behind larger sockets. All of this raises the stakes considerably.
The good news is that a healthy socket after wisdom tooth removal looks and behaves the same way as any other extraction site: a visible dark clot, decreasing pain, and gradual tissue coverage. The bad news is that the risk window is wider, pain is naturally higher at baseline, and it can be harder to self-assess because the site is harder to see.
Key differences for wisdom tooth recovery:
- Pain after wisdom tooth extraction is generally higher than a simple extraction — so the baseline is already uncomfortable
- The dry socket risk is higher here: studies estimate the rate of dry socket after wisdom tooth removal is significantly above the standard 2–5% for routine extractions
- The healing timeline is longer — gum closure can take 2 to 3 weeks, and full bone healing takes 2 to 3 months
If you are recovering from wisdom tooth removal and your pain spikes sharply after day 2 or 3 instead of gradually easing, do not dismiss it as “normal wisdom tooth pain.” That escalating pain pattern is the hallmark of dry socket, and it needs to be checked by a dentist.
Fact #11: According to Borda Family Dental, worsening pain two to four days after any extraction — but especially after wisdom tooth removal — should be evaluated by a dental provider, as it is the primary indicator of dry socket rather than normal healing.
Most dental professionals agree that once you pass the five-day mark after surgery — with pain decreasing and a clot still visible — you can feel reasonably confident that you are in healthy socket territory, not dry socket territory.
That said, if pain starts worsening at any point before that window closes, do not wait. Contact your dentist or oral surgeon promptly. Dry socket does not resolve on its own; professional treatment is necessary to manage the pain and support healing.
The simplest healthy socket vs dry socket rule: Pain should go down over time, not up. If it goes up, call your dentist.
How Is Dry Socket Treated?
If you have confirmed through symptoms that you are dealing with a dry socket rather than a healthy socket, the good news is that dry socket is treatable and not considered a life-threatening condition. Treatment is primarily focused on pain relief and protecting the exposed area so that healing can restart.
Your dentist will typically:
- Gently clean the socket to remove any food debris or bacteria
- Place a medicated dressing inside the socket — often containing numbing agents like eugenol or lidocaine
- Recommend pain relievers such as ibuprofen or acetaminophen for at-home management
- Prescribe antibiotics only if there are signs of active infection — dry socket itself is not an infection, so antibiotics are not always necessary
Fact #9: According to the Cleveland Clinic, with proper dental care, a dry socket typically heals within seven to ten days, during which time new tissue gradually covers the exposed bone.
Pain usually improves noticeably within 24 to 72 hours after the medicated dressing is placed. Follow-up appointments may be needed to change the dressing as healing continues.
How Can You Prevent Dry Socket?
The best way to keep yourself on the healthy socket vs dry socket right side of that comparison, is simple: protect the blood clot in those first critical days. Prevention is far easier than treatment, and most of the steps are straightforward.
Do:
- Follow all post-operative instructions from your dentist precisely
- Rinse gently with warm salt water as directed (usually starting 24 hours after the procedure)
- Stick to soft foods — yogurt, mashed potatoes, soup, and smoothies (consumed with a spoon) are ideal
- Keep your mouth clean with gentle brushing, avoiding the extraction site directly
Avoid:
- Straws for at least 5 to 7 days after extraction
- Smoking or any tobacco or vaping products
- Vigorous spitting or rinsing in the first 24 to 48 hours
- Fizzy or carbonated drinks while healing
- Hard, chewy, or crunchy foods until the socket is well-covered
Fact #10: The Cleveland Clinic explicitly lists avoiding straws, tobacco, and warm or fizzy drinks as key preventive steps after extraction — all due to the risk of dislodging the protective blood clot.
Summary: Healthy Socket vs Dry Socket
| Feature | Healthy Socket | Dry Socket |
|---|---|---|
| Appearance | Dark clot, no visible bone | Open, pale/gray, bone may be visible |
| Pain pattern | Decreasing each day | Worsening 1–3 days post-extraction |
| Smell/taste | Normal | Foul odor or bad taste |
| Healing timeline | 1–2 weeks for gum closure | Extended; requires dental treatment |
| Bone healing | Continues under gum | Delayed without intervention |
| Treatment needed | None; follow standard care | Yes — medicated dressing required |
Final Thoughts
Recovering from a tooth extraction is not always comfortable, but it follows a logical and predictable path when things go right. The entire healthy socket vs dry socket question really comes down to one thing: watch your pain trend. In a healthy socket, pain decreases each day. In a dry socket, it escalates. That single pattern — improving vs. worsening — is your most reliable guide.
You do not need to diagnose yourself perfectly. You just need to recognize the warning signs early enough to act on them. Bookmark this healthy socket vs dry socket guide, check your symptoms against it in the days after your extraction, and when in doubt, contact your dental provider. Dry socket is very treatable, and there is no reason to endure the pain alone.
Frequently Asked Questions
Can a dry socket heal on its own without treatment?
No. If you are dealing with a dry socket rather than a healthy socket, it will not resolve by itself. The exposed bone and nerves will continue to cause pain until a dentist places protective treatment. Delaying care only prolongs the discomfort and increases the risk of complications.
Is dry socket the same as an infection?
Not exactly. Dry socket is not an infection in the traditional sense — it is the result of a missing or dislodged blood clot, not a bacterial invasion. That distinction is also important for the healthy socket vs dry socket conversation: a healthy socket can sometimes look mildly inflamed without being infected, and a dry socket can exist without infection but still cause severe pain. Antibiotics alone are not effective for dry socket. However, an exposed socket can become secondarily infected if left untreated.
How long does dry socket pain last?
With treatment, pain typically improves within 24 to 72 hours and resolves fully within one to two weeks. Without treatment, the pain can persist for much longer and become increasingly difficult to manage.
Can you eat normally with dry socket?
It is highly advisable to stick with soft foods and avoid anything that requires chewing near the extraction site. Hard or chewy foods can aggravate the exposed bone and delay healing.